If you’ve been strength training for years and suddenly feel like your body isn’t bouncing back the way it used to, you’re not imagining it — recovery and strength training during menopause genuinely work differently than they did before.
Why Hormonal Shifts Rewrite the Rules of Recovery
To understand why recovery changes during menopause, you need to start with estrogen — a hormone most people associate with reproduction but that quietly does an enormous amount of work across almost every system in your body.
Estrogen plays a significant role in muscle repair, collagen production, regulation of inflammation, and even in how your nervous system responds to physical stress. When estrogen levels begin declining — typically starting in perimenopause, the transitional phase that can begin in your 40s — your body’s ability to recover from intense training is genuinely compromised. This isn’t a weakness. It’s biology.
Progesterone, another hormone that drops during this transition, has a calming effect on the nervous system. Lower progesterone means your body spends more time in a heightened state of stress, which directly impedes recovery. Add cortisol dysregulation (common during menopause) into the mix, and you have a situation where the same workout that used to leave you energized might now leave you depleted for days.
Understanding this hormonal context is the first step toward training smarter rather than just training harder.
How Menopause Changes Muscle, Bone, and Connective Tissue
Here’s something that doesn’t get discussed enough: menopause significantly accelerates muscle loss and bone density decline, making strength training more important than ever — but also more nuanced.
Estrogen acts as a mild anabolic signal in muscle tissue. It supports protein synthesis and helps blunt the breakdown that follows hard training sessions. When estrogen declines, muscle protein synthesis becomes less efficient, meaning your muscles don’t rebuild quite as quickly after being broken down by exercise. You need more protein, more recovery time, and smarter programming to achieve the same adaptive response.
Bone density is another major concern. The first five to seven years after menopause represent the period of fastest bone loss, driven largely by the drop in estrogen. Resistance training — particularly load-bearing exercises that place mechanical stress on bones — is one of the most evidence-backed ways to preserve and even rebuild bone density during this window. Skipping the gym isn’t the safe choice; it’s actually the riskier one.
Then there’s connective tissue. Collagen synthesis, which depends heavily on estrogen, slows considerably during the menopausal transition. Tendons and ligaments become less elastic and more prone to injury. This doesn’t mean you should avoid challenging loads, but it does mean you need to warm up more thoroughly, progress more gradually, and pay close attention to joint pain signals you might have previously pushed through.
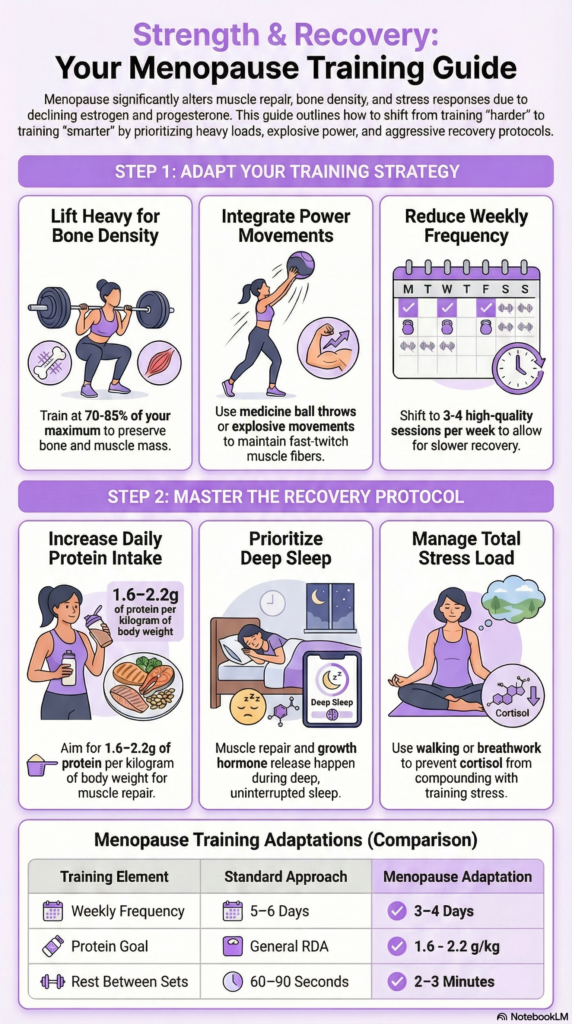
Strength Training During Menopause: What to Keep, What to Modify
The core principles of strength training don’t change during menopause — progressive overload, compound movements, and consistent effort still drive results. What changes is how aggressively you apply those principles and how much recovery bandwidth you build into your program.
Keep the heavy lifting. There is a persistent myth that women in midlife should shift entirely to light weights and high reps. The research does not support this. Heavy resistance training — working at 70 to 85 percent of your one-rep max — remains effective and is specifically valuable for preserving bone density and muscle mass during menopause. Compound lifts like squats, deadlifts, rows, and overhead pressing should stay in your programming.
Reduce training frequency if recovery is lagging. If you were previously training five or six days per week with high intensity, this may no longer be sustainable. Many women find that three to four sessions per week, with adequate rest between sessions, produce better results than cramming in more volume. The gains happen during recovery — if recovery is compromised, more training doesn’t help.
Prioritize session quality over quantity. A focused 45-minute session with full presence and effort will outperform a fatigued 90-minute grind. This is especially true when managing training for menopausal women, where hormonal factors can amplify the stress load of exercise if intensity is chronic or excessive.
Include power work. Studies suggest that fast-twitch muscle fibers decline more rapidly with age and are important for fall prevention and functional strength. Including some power-based movements — medicine ball throws, jump variations if joints allow, or explosive push movements — helps maintain neuromuscular speed and coordination.
Rethinking Recovery: Sleep, Protein, and Stress Load in Menopause
Recovery is never just about rest days. It’s a full-system process involving sleep, nutrition, stress management, and nervous system regulation — and menopause can disrupt each of these.
Sleep becomes both more important and harder to get. Night sweats and hot flashes frequently fragment sleep during perimenopause and menopause, which directly sabotages recovery. Deep sleep is when growth hormone is released, muscle repair accelerates, and the nervous system restores itself. Protecting sleep quality should be treated as a training priority, not an afterthought. This might mean adjusting your room temperature, limiting alcohol (which worsens night sweats), or speaking with a healthcare provider about options if sleep disruption is severe.
Protein requirements increase. To support muscle protein synthesis that is less efficient without adequate estrogen, many exercise physiologists recommend that menopausal women aim for 1.6 to 2.2 grams of protein per kilogram of body weight daily — higher than general guidelines. Spreading protein across meals rather than loading it all at dinner appears to optimize muscle building and repair. Don’t underestimate this variable. Inadequate protein is one of the most common reasons women in this phase plateau despite consistent training.
Manage total stress load, not just training stress. Your body processes all stressors through the same hormonal pathways. A high-stress workweek, poor sleep, undereating, and three hard training sessions don’t add up to a manageable week — they compound. Women in menopause often have less of a hormonal buffer to absorb this combined load. Practices like yoga, walking, breathwork, and deliberate downtime are not indulgences; they are recovery tools that support your ability to train hard when it counts.
Consider longer rest intervals between sets. Research on older athletes suggests that rest periods of two to three minutes between heavy sets — rather than the 60 to 90 seconds often recommended in general programs — may support greater strength expression and reduce excessive cortisol responses during sessions.
Common Mistakes Women Make with Strength Training After Menopause
Even with the best intentions, there are patterns that hold women back during this phase. Recognizing them is half the battle.
The most common is doubling down on cardio when strength training feels hard. Endurance work absolutely has a place, but chronic high-volume cardio without adequate resistance training accelerates muscle loss and does less for bone density. If you’ve been piling on HIIT classes or long runs, hoping to manage weight gain and mood shifts without a solid resistance-training foundation underneath, you may be working against yourself.
Another common mistake is ignoring soreness signals. Delayed onset muscle soreness (DOMS) tends to last longer and feel more intense during menopause due to slower repair processes. Pushing through excessive soreness too quickly increases the risk of injury and can create a cycle of chronic fatigue. If you’re regularly sore for four or five days after a session, that’s feedback — not a badge of honor.
Finally, many women fail to adjust their nutrition when they shift their training approach. Reduced estrogen changes how your body stores and uses fat, how it responds to carbohydrates, and how efficiently it builds muscle. Working with a registered dietitian who understands menopausal physiology can dramatically improve your results.
Conclusion
Strength training during menopause isn’t just still worth doing — it’s arguably more important than at any other phase of life. But to get the results you’re looking for, recovery needs to become a serious part of your strategy. The hormonal landscape has changed, and your approach should reflect that. Work with the biology rather than against it: prioritize protein, protect your sleep, manage your total stress load, and give yourself permission to recover more deliberately between sessions.
The women who thrive with strength training during menopause aren’t the ones who push hardest, regardless of how they feel. They’re the ones who understand that recovery is the work — and adjust accordingly.
Ready to build a strength program designed around your menopause transition? Book a consultation with a coach who specializes in training for women in perimenopause and menopause, and get a plan that actually fits where your body is right now.



