You’re doing everything right — eating well, staying active, managing your stress — and yet your body feels like it’s working against you. If you’re a woman over 40 experiencing unexplained weight gain, mood swings, brain fog, or sleep disruption, these aren’t random health problems. They’re perimenopause symptoms, and the hormone changes happening in your 40s are the reason no one has been able to give you a straight answer.
The frustrating part? Most women don’t get a warning. One day you feel like yourself, and the next you’re wondering why your jeans don’t fit the same way, why you snapped at your coworker over nothing, or why you’re lying awake at 3 a.m. staring at the ceiling. You’re not falling apart. Your hormones are shifting — and understanding why is the first step to feeling like yourself again.
What Actually Happens to Your Hormones in Your 40s
Perimenopause — the transition period before menopause — typically begins in a woman’s early to mid-40s, though it can start as early as 38. Most women don’t realize they’re in it because no one told them what to look for.
Here’s what’s happening beneath the surface.
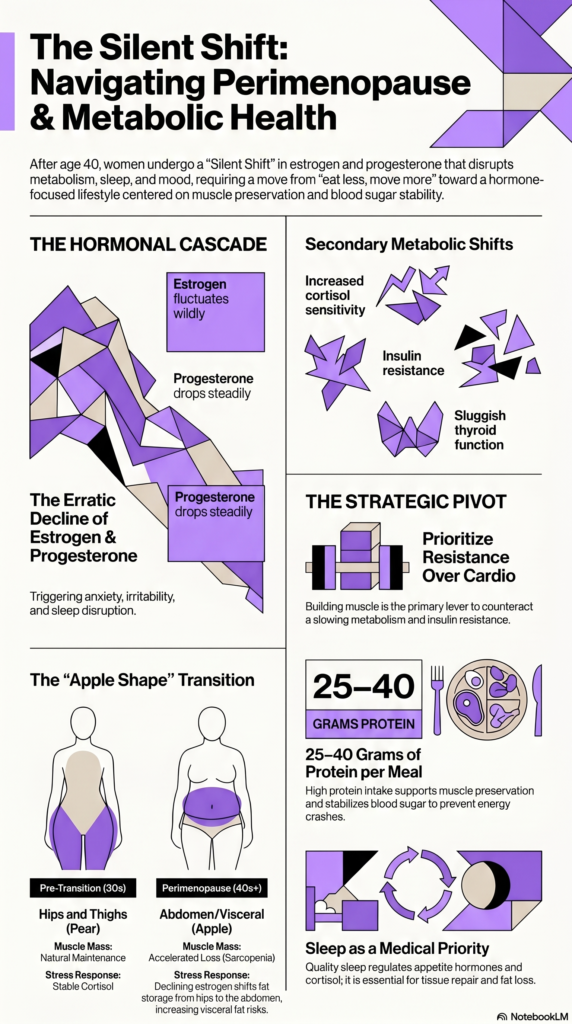
Your ovaries begin producing less estrogen and progesterone, the two hormones that have governed your cycle, mood, metabolism, sleep, and dozens of other functions since puberty. But this decline isn’t smooth or predictable. Estrogen fluctuates wildly before it drops, sometimes surging to levels higher than normal, then crashing — which is why your symptoms can feel so erratic and confusing.
Progesterone, on the other hand, tends to decline earlier and more steadily. Because progesterone is your calming, sleep-promoting hormone, this drop often shows up first as anxiety, irritability, and disrupted sleep — symptoms that look a lot like burnout or depression.
Meanwhile, your body is also experiencing shifts in:
- Cortisol sensitivity — your stress response becomes more reactive, making it harder to recover from everyday pressure
- Insulin regulation — your cells become less responsive to insulin, increasing the risk of blood sugar swings and belly fat accumulation
- Thyroid function — estrogen decline can influence thyroid hormone conversion, contributing to fatigue and sluggish metabolism
- Testosterone — yes, women have testosterone too, and a drop here affects libido, motivation, and muscle maintenance
This isn’t one hormone doing one thing. It’s a cascade — and it explains why perimenopause symptoms in women over 40 can look so different from woman to woman.
Why the Signs of Estrogen Decline Are So Easy to Miss
The medical system was not designed with the perimenopausal woman in mind. Most women are told their labs look “normal” when their symptoms are very real. Here’s why that happens.
Standard hormone panels often test estrogen at a single point in time. But because estrogen fluctuates so dramatically during perimenopause, a one-time reading can look perfectly fine even when your levels are swinging dramatically throughout the month. This is one of the most common reasons women are dismissed — or misdiagnosed with anxiety, depression, or thyroid issues — when the root cause is hormonal.
The signs of estrogen decline are often mistaken for other conditions. Brain fog gets chalked up to stress. Weight gain around the midsection is blamed on a poor diet. Sleep problems are attributed to screens or a busy schedule. Mood changes are labeled as anxiety or burnout.
Here’s a list of symptoms that are commonly connected to the estrogen and progesterone shift — many of which women never associate with their hormones:
- Difficulty concentrating or remembering words (brain fog)
- Waking between 2–4 a.m. and struggling to fall back asleep
- Increased anxiety or a sense of dread without a clear cause
- Irregular or heavier periods
- Hot flashes or night sweats
- Unexplained weight gain, especially around the abdomen
- Decreased motivation or feeling emotionally flat
- Joint pain or increased muscle soreness
- Skin changes — dryness, loss of elasticity
- Low libido
You don’t need to have all of these. Even three or four of these symptoms in a woman over 40 is worth paying attention to. Your body is communicating. The goal is to learn how to listen.
How Hormone Changes in Your 40s Affect Your Metabolism and Body Composition
This is the section most articles skip — and it’s the one that explains why what worked before no longer works now.
Estrogen plays a direct role in how your body stores fat. When estrogen is abundant, fat tends to be stored in the hips and thighs — the classic “pear shape.” As estrogen declines, fat storage shifts toward the abdomen — the “apple shape” — which is not just a cosmetic change. Visceral fat, the fat stored around your organs, is metabolically active and is associated with increased inflammation, insulin resistance, and cardiovascular risk.
This is why the scale can go up even when your calorie intake hasn’t changed. This is why the diet that worked at 35 isn’t working at 44. It’s not a willpower problem. It’s a physiological problem.
At the same time, the decline in estrogen accelerates muscle loss — a process called sarcopenia. Muscle is your primary calorie-burning tissue. Less muscle means a slower metabolism. And without the right type of exercise to counteract this, the cycle compounds year after year.
Here’s what this means practically:
- Cardio alone won’t cut it. Hours on the treadmill may actually increase cortisol, which worsens the hormonal picture.
- Caloric restriction backfires. Eating too little signals your body to hold onto fat stores and breaks down muscle for energy.
- Strength training becomes non-negotiable. Building and preserving muscle is the most powerful metabolic lever you have in perimenopause.
- Blood sugar stability matters more than ever. Erratic eating patterns that trigger insulin spikes accelerate fat storage and energy crashes.
A client I worked with — a 46-year-old attorney — came to me frustrated and exhausted. She was running four days a week and eating what she considered a clean diet. She’d gained twelve pounds in a year and couldn’t sleep more than five hours. When we looked at her patterns, she was undereating protein, skipping meals under deadline pressure, and doing steady-state cardio that was spiking her cortisol.
Within eight weeks of adjusting her training, eating more — not less — and prioritizing sleep hygiene, she lost six pounds and reported sleeping through the night for the first time in months.
The hormone changes in your 40s aren’t a sentence. They’re a signal to change your strategy.
What You Can Actually Do About Perimenopause Symptoms Right Now
Understanding why this is happening is empowering. But you also need a path forward.
Here are the evidence-based areas that make the biggest difference for women managing perimenopause symptoms without medication:
Prioritize Protein at Every Meal
Most women eat far too little protein — especially in the morning. Protein supports muscle preservation, helps regulate blood sugar, and keeps you fuller longer. Aim for 25–40 grams per meal. Think eggs and Greek yogurt at breakfast, not just a smoothie or piece of toast.
Shift Your Exercise Strategy Toward Resistance Training
This doesn’t mean giving up walking or yoga. It means adding two to three sessions per week of intentional strength training that challenges your muscles. Compound movements — squats, deadlifts, rows, presses — do the most for metabolism and hormone-sensitive tissue.
Address Sleep as a Medical Priority, Not a Luxury
The decline in progesterone directly disrupts sleep architecture. Improving sleep isn’t just about rest — it directly affects cortisol, insulin, appetite hormones (ghrelin and leptin), and your body’s ability to repair tissue. A consistent sleep window, reduced alcohol, a cooler room, and magnesium glycinate before bed are starting points.
Reduce Inflammatory Foods, Not Just Calories
Processed carbohydrates, refined seed oils, sugar, and alcohol all increase systemic inflammation, which amplifies every perimenopause symptom. An anti-inflammatory eating pattern built around whole foods, healthy fats, and quality protein creates the internal environment your hormones need to stabilize.
Work With Someone Who Understands This Transition
This is where generic advice runs out. Every woman’s hormone picture is different. Her stress load is different. Her training history is different. Her relationship with food is different. A personalized approach — not a one-size-fits-all program — is what moves the needle.
If you’re working with women in Charlotte or coaching clients globally online, the need is the same: someone who will look at your whole picture and help you build a strategy that fits your actual life.
Common Mistakes Women Make When Managing Hormone Changes After 40
Before you go and adjust everything at once, it’s worth naming the traps that slow progress.
Trying to out-exercise a hormonal problem. More cardio, more restriction, more effort — without the right strategy — often worsens cortisol and makes symptoms worse.
Waiting until symptoms are severe to seek support. The earlier in perimenopause you address these shifts, the more leverage you have. Waiting until menopause often means playing catch-up.
Relying on general wellness content. Generic advice doesn’t account for your unique hormone picture, your health history, or the specific patterns driving your symptoms.
Going it alone. The women who navigate this transition most successfully are those who have expert guidance and community support — not just information.
FAQ: About Perimenopause Symptoms and Hormone Changes
How do I know if I’m in perimenopause?
Perimenopause is diagnosed based on symptoms and age, not a single lab test. If you’re a woman over 40 with irregular cycles, sleep disruption, mood changes, or unexplained weight gain, it’s worth having a conversation with your provider — and potentially a health coach who specializes in this transition.
Can perimenopause start in your late 30s?
Yes. While the average onset is in the early to mid-40s, some women begin experiencing perimenopause symptoms as early as 38. If your symptoms are present and your doctor hasn’t connected them to hormones, push for a more thorough conversation.
Do I need hormone replacement therapy to manage perimenopause?
Not necessarily. Many women manage their symptoms effectively through targeted lifestyle changes — nutrition, strength training, stress management, and sleep optimization. That said, HRT is a valid medical option for some women, and that conversation belongs with your doctor.
Why am I gaining weight even though I’m eating the same as always?
The decline in estrogen changes where and how your body stores fat. Combined with shifts in insulin sensitivity and muscle loss, your metabolism is operating differently than it did at 35. Calorie math alone doesn’t account for these hormonal shifts.
What’s the difference between perimenopause and menopause?
Perimenopause is the transition phase — the years of fluctuating hormones and irregular cycles leading up to menopause. Menopause is a single point in time: 12 consecutive months without a period. Most women spend 4–10 years in perimenopause before reaching that milestone.
You Don’t Have to Figure This Out Alone
Your body changing after 40 isn’t a failure. It’s a transition — and, like any major transition, it goes better with the right support and strategy.
You deserve more than a list of tips. You deserve a plan built around your life, your hormones, and your goals — one that actually accounts for the complexity of what you’re experiencing.
If you’re ready to stop guessing and start getting answers, explore personalized 1-on-1 coaching designed specifically for high-achieving women navigating perimenopause. Women in Charlotte, NC and around the world are doing this work — and feeling like themselves again.



